By: Jake Smiths
The American healthcare industry is at a critical inflection point. For decades, it has been shaped by incentives that reward volume over sustained wellness. As a result, chronic diseases dominate both health outcomes and spending. Yet, just as nutrition science is recalibrating long‑held assumptions about what we eat, a new wave of preventive‑first thinking is reshaping how care might be delivered.
At the forefront of this emerging philosophy is Longevitix, a healthspan‑focused preventive care intelligence platform that believes the next foundational framework for healthcare should be a “preventive pyramid” that flips care on its head.
The Reality of America’s Health Burden
The latest data from the U.S. Centers for Disease Control and Prevention reveal that ultra‑processed foods, industrialized products high in sugar, salt, and refined carbohydrates, now make up 55 % of total calories consumed by Americans age 1 and older, with children consuming nearly 62 % of their daily calories from such foods. These dietary patterns, linked to obesity, Type 2 diabetes, heart disease, and other chronic conditions, underscore how misaligned basic lifestyles are with human biology and long‑term health.
This dietary imbalance mirrors what many experts see in the healthcare system. Chronic diseases, like cardiovascular disease, diabetes, and obesity, are not rare outliers; they are the dominant source of morbidity, mortality, and cost in the United States. According to public health data and expert analysis, chronic conditions account for a significant share of overall healthcare spending in the United States, which totals several trillion dollars annually, even as preventive care utilization remains relatively low.
Despite well‑established clinical guidelines for prevention, only a small fraction of adults receive full evidence‑based preventive services. A prior national review found that only a small percentage of U.S. adults received all recommended preventive screenings and services, while a notable portion received none.
This gap highlights not just a failure to use effective tools, but a broader systemic disincentive: a healthcare model built around reacting to disease rather than preventing its onset.
From Static Snapshots to Continuous Signals
Traditional healthcare, much like the decades‑old food pyramids, has relied on episodic, snapshot assessments. Annual check‑ups, one‑off screenings, and clinic visits provide intermittent windows into a patient’s health. But biology doesn’t work in discrete intervals. Physiological changes such as metabolic drift, inflammation, and early organ dysfunction accumulate gradually, often long before symptoms appear.
This is where digital biomarkers enter the conversation. Defined as quantifiable physiological and behavioral data captured through wearables, biosensors, and mobile technology, digital biomarkers enable continuous real‑world monitoring of health signals.
The digital biomarkers market is rapidly expanding, driven by advances in wearable sensors, smartphone platforms, and AI‑powered analytics that can detect subtle changes in heart rate, sleep patterns, activity levels, and other metrics long before traditional clinical thresholds are crossed.
This shift from static checks to dynamic, longitudinal tracking enables a fundamentally different approach: one that anticipates risk and intervenes before disease becomes clinically manifest, rather than waiting to react once a condition has taken root.
Reimagining the Healthcare Pyramid
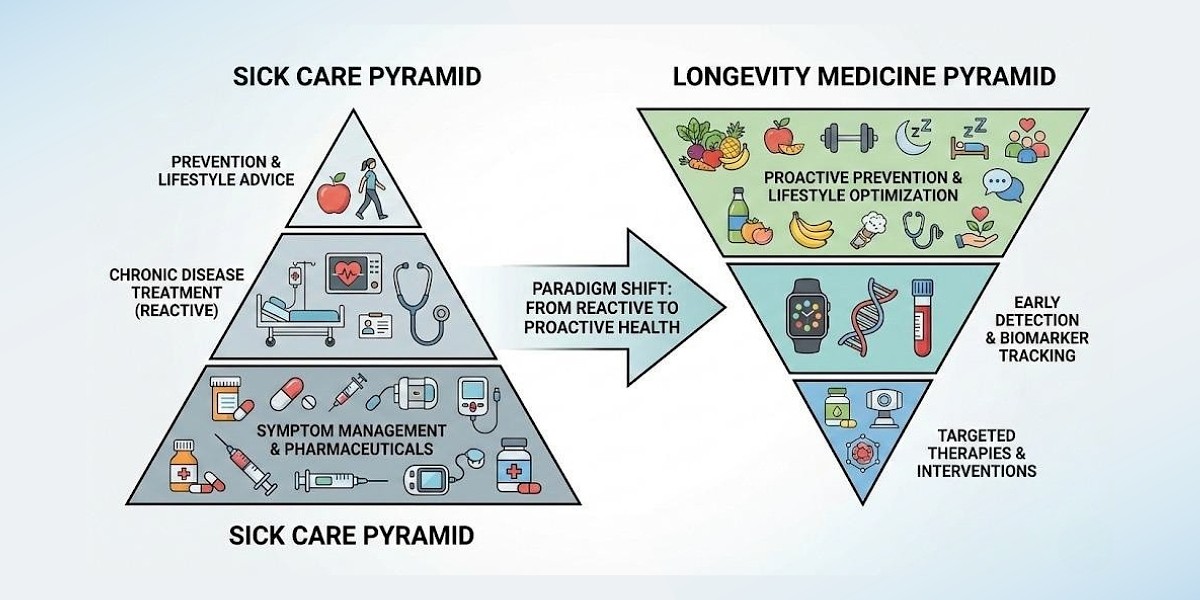
Longevitix’s recently unveiled preventive pyramid reframes how care should be organized. In traditional models, symptom management and pharmaceuticals sit at the base, with lifestyle advice and prevention relegated to the narrow apex, a reflection of how care is actually delivered today.
In contrast, the Longevitix preventive pyramid places proactive prevention and lifestyle optimization at its foundation. Above that is continuous biomarker tracking for early detection. At the top, reserved for targeted therapies, are interventions deployed precisely and sparingly, informed by longitudinal, personalized biological data.
This restructuring mirrors how modern nutrition science is moving beyond one‑size‑fits‑all food pyramids to guidance rooted in metabolic reality, emphasizing whole, nutrient‑dense foods over ultra‑processed foods that dominate current consumption patterns.
The implication for healthcare is profound. By stacking the system to prioritize prevention and early insight, Longevitix’s model seeks to shift economic incentives away from high‑volume treatments and toward maintaining physiological stability over time.
Aligning Incentives With Biology, Not Billing Codes
Both food policy and healthcare reform face similar challenges: entrenched incentives that prioritize efficiency and scale over biology‑centric outcomes. For nutrition, this has meant cheap, shelf‑stable foods feeding a chronic disease epidemic. In healthcare, it has meant that expensive late‑stage treatment has dominated expenditure.
Investing in prevention, from diet and lifestyle interventions to early risk detection, isn’t just a health ideal; it’s an economic strategy. Research suggests that increasing uptake of preventive services can reduce the burden of chronic disease, and continuous monitoring using digital biomarkers shows promise for identifying risk patterns earlier than traditional models allow.
Longevitix’s approach does not replace clinical care but complements it by providing clinicians with data‑driven, personalized insights that can inform decisions long before conventional symptoms demand attention.
A New Organizing Principle for Healthspan
Redesigning healthcare for biology rather than crisis response won’t be easy. It requires aligned incentives, robust technology, clear evidence, and cultural buy‑in from providers and patients alike. But the conceptual blueprint now emerging, informed by advances in biomarkers, data science, and personalized monitoring, suggests a fundamentally different future.
If healthcare can evolve from episodic reaction to continuous prevention, the benefits could be transformative: reduced disease burden, lower costs, and most importantly, longer, healthier lives. Longevitix’s preventive pyramid is not just a visual shift; it represents a philosophical reorientation that could define healthcare for the next decade and beyond.
Disclaimer: This article is for informational and educational purposes only. It does not constitute medical, financial, or investment advice. Any references to health technologies, preventive strategies, or economic impact are based on publicly available information and industry perspectives. Readers should consult qualified healthcare professionals before making decisions related to medical care or health interventions.