By: Siegfried and Jensen
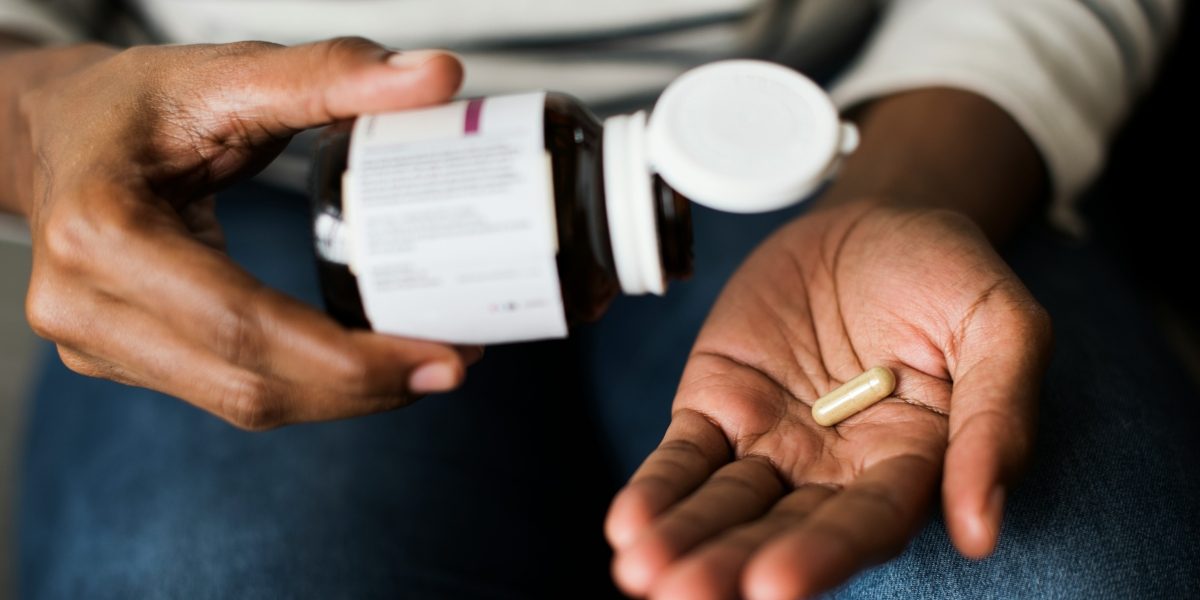
Medication errors remain a persistent and preventable danger in American healthcare, with significant consequences for patients. A new analysis from Siegfried & Jensen sheds light on the ongoing issue in New York. From misprescribed antibiotics to high-risk cardiovascular drugs, the study reveals that thousands of patients, especially seniors, are at risk each year due to improper prescribing, dispensing, or medication management.
Across the U.S., it is estimated that at least 1.5 million Americans suffer harm annually from medication errors, with thousands of deaths occurring each year as a direct result. While statistics on exact death tolls vary, studies suggest that between 7,000–9,000 deaths may occur annually due to medication errors, though some reports estimate this number could be higher, depending on definitions and underreporting. Alarmingly, many errors stem from the prescription stage, where at least 91% of errors have been reported in some studies, though figures may vary based on methodologies used.
New York: A Hotspot for High-Risk Medication Oversight
New York, with one of the largest senior populations in the U.S., is particularly vulnerable to medication errors. The state’s pharmacies handle high prescription volumes, which increases the likelihood of dispensing mistakes, rushed verification, and lapses in oversight. In 2024, New York recorded 61 disciplinary actions against pharmacists, placing it among the top 10 states for adverse pharmacy reports.
The state’s challenges are compounded by its dense population and large elderly demographic. The combination of polypharmacy (patients using multiple medications) and high pharmacy workloads contributes to an environment where small oversights can escalate into serious medical emergencies.
The Drugs Most Commonly Involved in Medication Errors
Siegfried & Jensen’s analysis identifies several medication categories that are frequently involved in errors both in New York and across the nation:
- Antibiotics (20%): Frequently misprescribed due to strict dosing requirements and their widespread use.
- Antipsychotics (19%): High-risk medications that require close monitoring, particularly for patients with severe mental illness.
- Central Nervous System (CNS) drugs (16%): Including anti-seizure and sleep medications, these drugs often have complex dosing schedules.
- Cardiovascular medications (15%): Essential for chronic care but highly sensitive to dosage errors.
- Opioids (7%): Although less frequent, errors involving opioids can be fatal.
In New York, where chronic illnesses and polypharmacy rates are high—particularly among older adults—the margin for error is small.
Who Faces the Greatest Risk?
Certain populations in New York are especially vulnerable to medication errors:
- Older Adults: Nearly 40% of Americans aged 65+ take five or more medications. Those on multiple prescriptions are at a higher risk of harm from medication errors.
- Individuals with Mental Health Conditions: Antipsychotic medications contribute to nearly 1 in 5 medication errors. A significant percentage of people with severe mental illness misuse or mismanage their prescriptions.
- Children: Pediatric medication errors often result from labeling misunderstandings or mismeasured dosages.
The risk is amplified in high-density areas like New York, where busy hospital systems, crowded clinics, and high-volume pharmacies serve diverse populations.
The Common Types of Medication Errors
Medication errors can happen at various points in care, from prescription to administration:
- Wrong timing (33.6%): Especially dangerous for antibiotics and blood thinners.
- Wrong dose (24.1%): One of the leading causes of complications.
- Wrong medication (17.2%): Often linked to similar-sounding or -looking drug names.
- Pharmacy dispensing errors: Includes wrong strength, quantity, or mislabeled packages.
- Look-alike/Sound-alike (LASA) errors (25%): Among the most dangerous errors in both hospital and pharmacy settings.
These errors can lead to serious consequences, including seizures, cardiac events, internal bleeding, organ failure, anaphylaxis, and, in some cases, fatal overdoses.
Why Medication Errors Continue: Systemic Causes
The analysis identifies common causes behind medication errors, many of which stem from systemic issues:
- Illegible or incomplete prescriptions
- Missing patient allergy or medical history information
- Inadequate double-checking protocols
- Rushed pharmacist verification due to understaffing
- Poor communication between healthcare providers
A recent national survey cited in the study found that 80% of pharmacists link medication errors directly to staffing shortages—a significant concern in high-volume states like New York.
The Human and Financial Cost
Medication errors cost the U.S. healthcare system over $20 billion annually, and when factoring in long-term care, readmissions, and lost productivity, the economic burden may reach up to $77 billion. For patients and families, the costs are more personal: long-term disability, financial hardship, and, in the worst cases, the loss of life.
A Path Forward
Preventing medication errors requires coordinated action across the healthcare system. Some key steps toward improvement include:
- Standardized, electronic prescribing
- Clearer labeling and better patient instructions
- More robust pharmacy staffing and oversight
- Improved communication between doctors, pharmacists, and caregivers
- Greater public awareness around high-risk drugs
Medication safety is a shared responsibility. Strengthening safeguards, particularly in high-volume states like New York, can significantly reduce preventable harm and protect patients from potentially life-threatening errors.
Disclaimer: The information provided in this article is for general informational purposes only. The opinions expressed are those of the author and do not necessarily reflect the views or opinions of the publisher. The content includes branded information and may contain estimates or generalized data based on available research. While every effort has been made to ensure the accuracy of the information, the article should not be considered a substitute for professional medical or healthcare advice. Always consult with a qualified healthcare provider for advice regarding specific medical conditions or concerns.